A Spanish study of drug-induced eosinophilia found that early hypogammaglobulinemia was associated with subsequent HHV-6 reactivation in patients with severe drug hypersensitivity syndromes. This study of 274 cases out of 164,379 hospital admissions at La Paz University Hospital in Madrid confirms earlier reports from Japan and France that described transient reductions of total IgG at the outset of drug hypersensitivity reactions leading to HHV-6 reactivation.
The group found that high levels of eosinophilia were predictive of severe drug reaction, a condition known as eosinophilia and systemic symptoms (DRESS) or drug induced hypersensitivity syndrome (DIHS). Gammaglobulin levels were measured at the onset of symptoms before the administration of steroids. In cases where hypogammaglobulinemia was detected, there was a strong association with HHV-6 reactivation (R=0.931; p<0.001).
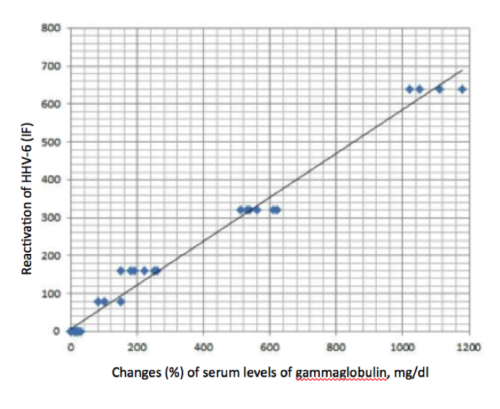
HHV-6 reactivation correlated with the change in total IgG. Source: British Journal of Clinical Pharmacology.
Most of the patients were already hospitalized when they developed the reaction, and the rest were admitted specifically for drug reaction. 56% of cases with drug-induced eosinophilia were asymptomatic, but 23% had severe symptoms associated with DRESS. The median number of days between drug administration and symptom appearance was 11 days for fever, 12 days for hypogammaglobulinemia, 21 days for eosinophilia, and 23 days for exanthema.
The incidence of drug related eosinophilia was rare, at only 16.67 per 10,000 hospital admissions. Treatment with corticosteroids resulted in significantly decreased eosinophils.
An earlier Japanese study (Kano 2004) also reported a significant increase in total IgG levels between the time of admission and upon recovery (p=0.005). The authors suggested that drugs, especially those with immunomodulatory effects on B cells, might cause transient hypogammaglobulinemia in these patients, activating the virus. However, a study the following year (Nakashima 2005) showed that hypogammaglobulinemia returned in a late flare long after the drug was discontinued, suggesting that the disease process might be causing the hypogammglobulinemia.
A 2006 French study compared 39 consecutive patients with DRESS to 52 patients with other causes of rash in the same period, and hypogammagolubinemia was significantly associated with DRESS (p=0.022) (Boccara 2006)
French dermatologist Vincent Descamps has proposed that dermatologists consider treating the HHV-6 (and CMV/EBV) reactivation with antivirals and notes that many transplant and emergency room patients develop symptoms of DRESS without a drug trigger. He calls this syndrome VRESS or “Virus Reactivation with Eosinophilia and Systemic Symptoms” (Descamps 2013).
Eosinophilia is typically defined as >700 cells/ μL. Levels of ≥1500/μL are associated with organ damage. The Spanish group found that 90% of the drug hypersensitivity cases came from adults and 10% were in children. Overall, only 8.5% of all eosinophilia was attributed to adverse drug reactions. The highest incidence of eosinophilia was seen during convalescence from viral, bacterial, or protozoal infections (19.6%), in preterm neonates (19.3%), and in cases of solid malignancies (11%), hematologic diseases (5.4%) and allergic disorders (5.4%).
The authors recommend that patients with highly elevated eosinophilia be followed closely at the outset of symptoms so that early diagnosis can be achieved.
For more information, read the full paper (Ramirez 2016) and visit the HHV-6 Foundation’s webpage on HHV-6 & Drug Hypersensitivity.