The severity of DIHS/DRESS cases was significantly correlated with the frequency of CD134+ cells.
Drug-induced hypersensitivity syndrome (DIHS)/drug rash with eosinophilia and systemic symptoms (DRESS) is a drug-induced delayed hypersensitivity reaction, one of several drug-induced severe skin (and systemic) reactions. DIHS/DRESS has been associated with reactivation of HHV-6B, and the viral reactivation is suspected of contributing to the course of severe organ disease.
HHV-6B uses CD134 as its primary receptor. CD134 (also called OX40) is a member of the tumor necrosis factor receptor superfamily. It has been previously shown that in DIHS/DRESS there is an increased number of CD134+ T cells in the peripheral blood, but not an increased number of T cells with other activation markers such as CD69 and CD25. Also, CD134 is upregulated preferentially in DIHS /DRESS with CD134 positivity previously found to be 23% of DIHS/DRESS patients compared to only 7% in Stevens Johnson Syndrome and 3% in maculopapular rash patients (Miyagawa 2016).
Investigators from Showa University School of Medicine in Tokyo, Japan, examined the presence of CD134+ T cells in both the peripheral blood and, using immunohistochemistry, in the dermis of 21 people with DIHS/DRESS, and compared the results to those seen in 11 patients with erythema multiforme, another inflammatory skin condition. They report finding CD134+ T cells much more frequently in the dermis of people with DIHS/DRESS than in those with erythema multiforme, as shown in Figure 1.
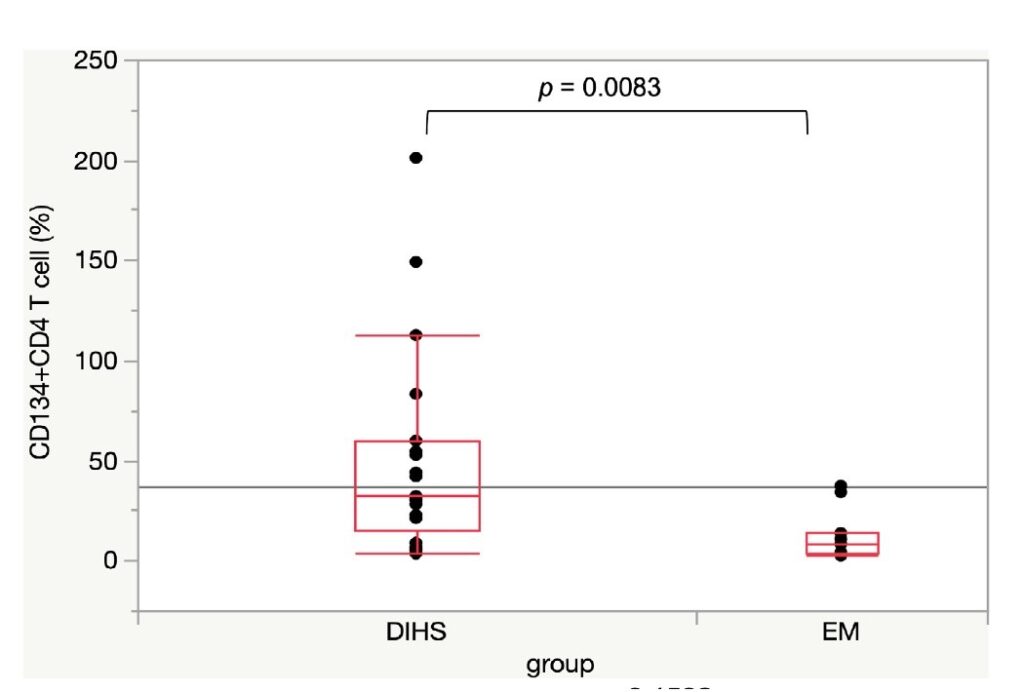
Figure 1 - Number of CD134+ cells in the dermis of patients with DIHS/DRESS vs. erythema multiforme (EM).
The investigators also report that the number CD134+ T cells in the dermis correlated with the DIHS/DRESS severity score (P=0.028), as shown in Figure 2, as well as with the frequency of HHV-6 reactivation (although the latter correlation was not statistically significant). Finally, they found that many of the CD134+ T cells in the dermis also stained positively for markers of T regulatory T cells.
The finding of increased numbers of CD134+ T cells in the dermis of patients with DIHS/DRESS indicates there are more cells capable of being infected by HHV-6B, or that already are infected with HHV-6B. However, staining with anti-HHV-6 (Abcam, 1:100) antibodies did not clearly reveal the presence of the virus in the dermis of people with DIHS/DRESS. The sensitivity of this assay is not reported.
The positive correlation of CD134+ T cells and DIHS/DRESS severity score suggests HHV-6B may contribute to the progression of DIHS/DRESS in some patients.
One theory proposed for the preferential reactivation of HHV-6B in the plasma of DIHS/DRESS patients is that the HMGB-1 released from damaged skin chemoattracts HHV-6 infected monomyeloid precursor cells to the skin where they interact with CD4 cells that then become infected (Hashizume 2013).Consistent with that theory, French dermatologists led by Vincent Descamps recently found HHV-6B in the skin a full two weeks before it was found in the blood. (Marcombes 2023).
Larger studies with more sensitive assays may be required to clarify the contribution of HHV-6B to DIHS/DRESS severity and progression.
Read the full article: Lee 2023