While the controls were negative, alcoholics were positive for HHV-6 in both white and gray matter.
Jain et al. (2021) of the Rīga Stradiņš University investigated the interaction of chronic alcoholism and HHV-6 in the promotion of neuroinflammation within the substantia nigra (SN), a region in the basal ganglia. Samples from 44 total autopsies were grouped into healthy (n=13, group A), age-matched alcoholics (n=13, group B), and chronic/non-age matched alcoholics (n=18, group C) and analyzed for several markers of microglia, particularly activated microglia (CD68, CD11b, and Iba1). HHV-6A/6B infection was detected with dual antibody immunohistochemistry.
The two alcoholic groups had significantly fewer perivascular CD68+ cells, but significantly more non-perivascular CD68+ cells, in the substantia nigra. There was a significant decrease in CD68 positive (CD68+) cells in the gray matter of SNpr between groups A and C (p=0.025). In the white matter of SNpr, there was a significant decrease of CD68+ between controls and alcoholics (Groups A/C p=0.000; Groups B/C p=0.021). In SNpc white matter, alcoholics showed significantly fewer CD68+ cells than controls (Groups A/B, A/C p = 0.003, 0.027), perivascularly. In perivascular SNpr, both alcoholic groups showed a decrease in CD68+, with group C having an even more precipitous drop in CD68+ (p<0.001). Conversely, alcoholic groups showed an increase in diffuse (not perivascular) CD68+ cells when compared with controls in both gray and white matter.
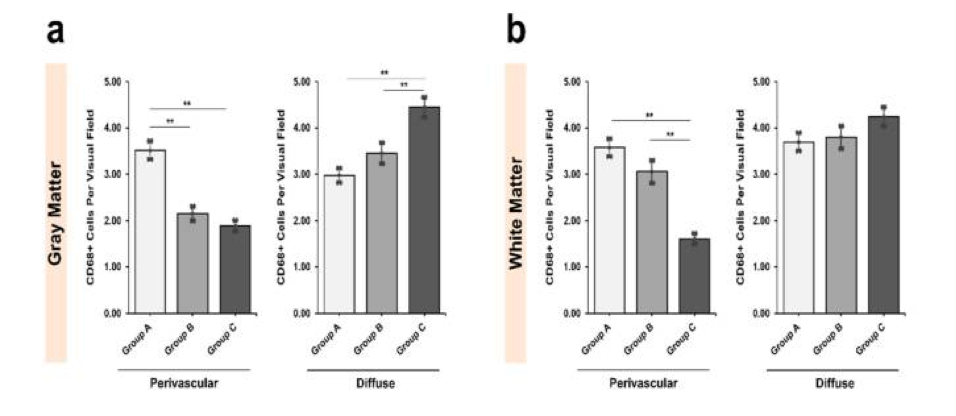
Comparison of diffuse and perivascular CD68+ in Pars Reticulata (SNpr) of the substantia nigra, for three studied groups, including both grey and white matter.
In terms of HHV-6 presence, none of the control individuals tested positive. 25% (8/31) in the alcoholic groups (B and C) were found to be positive for HHV-6B, but not HHV-6A. Among subjects who were HHV-6B+, there was a significant increase in Iba1+ cells, compared to both HHV-6 negative alcoholics and controls (panel b, below).
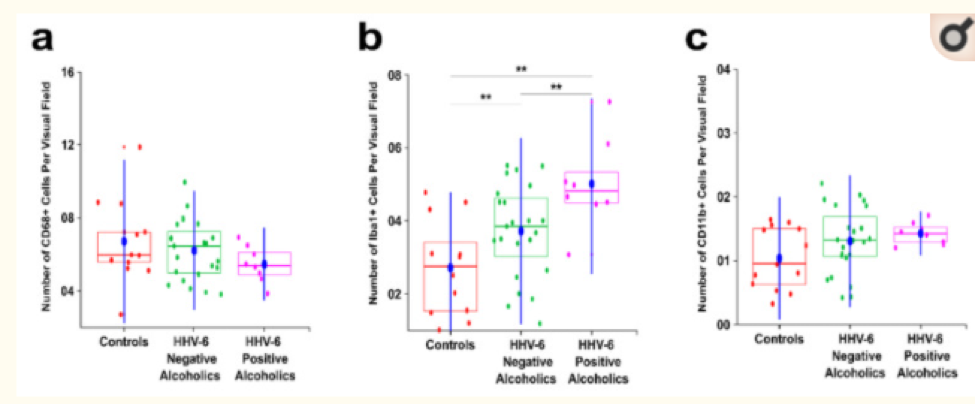
Comparison of CD68+, Iba1+, and CD11b+ cells between controls, HHV-6B- alcoholics, and HHV-6b+ alcoholics.
The significance in Iba1 differences points to HHV-6 and alcoholism interacting to produce greater levels of neuroinflammation.
Limitations of this study included its relatively small size, and somewhat inconsistent results between various markers of microglial activation.
Read the full article: Jain et al 2021

