A review of post-transplant cases found that the incidence of HHV-6 myelitis was 4.1%; symptoms of pruritus without rash, pain, numbness, dysuria and constipation are potential signs.
Japanese investigators from Keio University School of Medicine reviewed 19 patients over 15 years who developed HHV-6 myelitis after allogenic HCT and found a cumulative incidence of 4.1%. Notably, in all cases, myelitis developed within 1 month of the transplant. The most common symptoms at the onset of myelitis were pruritus (n=10) and pain (n=8). Less common symptoms included numbness and dysuria or constipation.
In three cases, myelitis was followed by the development of encephalitis, all marked by CSF HHV-6 DNA exceeding 10,000 copies/mL before the onset of encephalitis. These cases also had a significantly greater median copy number of HHV-6 in the CSF compared to cases of HHV-6 myelitis alone (40,000 copies/mL vs 2,000 copies/mL). No cases of HHV-6 myelitis developing after HHV-6 encephalitis were found.
Similar to HHV-6 encephalitis, the investigators reported that cord blood transplantation and mismatched donors were significant factors for the development of myelitis. They note that the prognosis of HHV-6 myelitis is more favorable than that of HHV-6 encephalitis, though recognizing that the incidence of HHV-6 myelitis alone is lower. In all cases, patients recovered with traditional treatments of foscarnet, ganciclovir, or both. Two developed neurological sequelae.
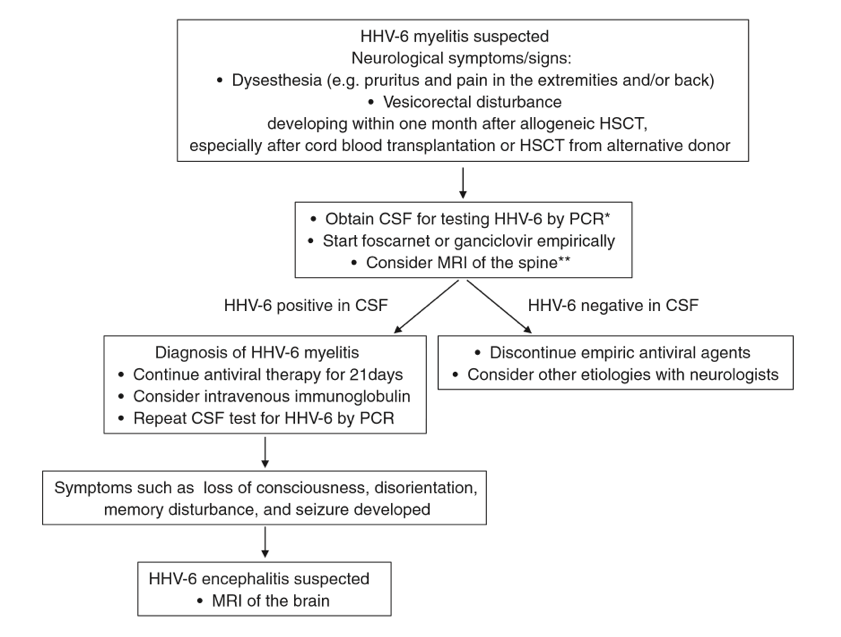
Currently, diagnostic criteria for HHV-6 myelitis are not well defined, though this study as well as others primarily base the diagnosis on myelitis symptoms with HHV-6 presence in the CSF or in some cases, the blood. Additionally, early management of HHV-6 myelitis may also help prevent the development of HHV-6 encephalitis. Below is a flowchart of their recommendations for the diagnosis and management of HHV-6 myelitis following alloHSCT.
Read the full-text: Shiroshita 2019